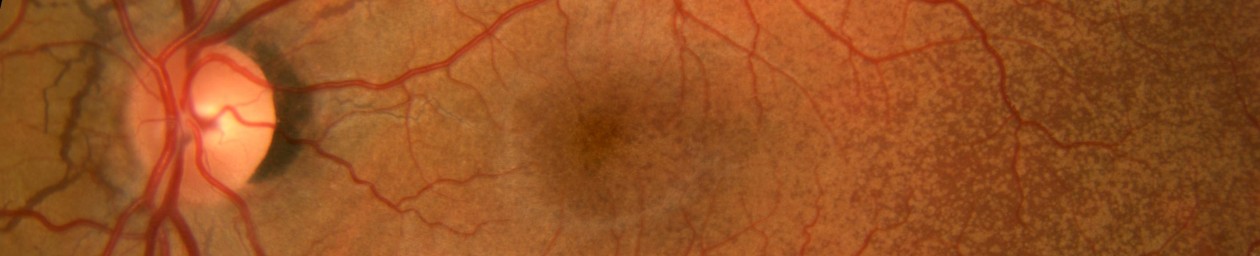
Fundus photography is a diagnostic imaging procedure that documents the clinical appearance of the retina, choroid, and optic nerve. It is the foundation for the profession of ophthalmic imaging. Fundus photography dates back to the late 1800’s when Jackman and Webster first described a technique for photographing the human retina. Today it continues to play a vital role in the documentation, diagnosis and treatment of retinal disorders.
Clinical Uses

Fundus photographs are used for clinical documentation, teaching, retinal screening, and remote consultation. Serial photographs are commonly used to track disease progression. Some retinal details may be easier to identify in stereoscopic fundus photographs compared with direct examination. Clinical trials rely on sophisticated photographic grading scales to confirm patient eligibility, classify disease severity and track the efficacy of treatment. Fundus photographs are also used as a baseline to assist in interpretation of other diagnostic imaging procedures such as fluorescein angiography.
Instrumentation

The modern fundus camera is a horizontally mounted instrument with an internal electronic flash and an attached 35mm camera or digital sensor. Fundus photography relies on the interaction between the optics of the fundus camera and the optics of the subject eye. Fundus cameras employ an aspheric optical design to match the plane of focus to the curvature of the fundus.

A viewing angle of 30-35 degrees is considered standard. Fixed-angle cameras usually offer the sharpest optics, but variable-angle cameras provide wide-angle capabilities between 45 and 60 degrees.
When equipped with appropriate filters, fundus cameras can also be used for fluorescein angiography, monochromatic photography, fundus autofluorescence imaging and indocyanine green angiography.
Illumination
The light needed to illuminate the fundus is delivered axially through the image-forming optics of the fundus camera. The optical system of the fundus camera projects a ring of light from the internal strobe through the dilated pupil. The ring shape allows a separation of the outgoing and incoming illumination. The ring fills the outer pupil with light that reflects off the retina, exits the pupil through the center of the ring, and continues through the optics of the fundus camera to form an image of the fundus at the film plane.

The fundus camera is equipped with a variable power incandescent viewing lamp to allow the operator to view the fundus for alignment and focus before exposure. A xenon-filled flash tube delivers a brief burst of intense light to expose the photograph. Pharmacologic dilation is necessary to obtain adequate illumination. Wide-angle cameras need to illuminate a large area of retina, requiring a more-widely dilated pupil to accommodate a larger ring of light.
Focus
Successful fundus imaging relies on the interaction between the optics of the fundus camera with the optics of the eye itself. Although the fundus camera is essentially a low-power microscope placed just an inch or two from the subject, proper focus is set at or near infinity, because when aimed into the eye, the light path exiting the fundus camera then passes through the refracting optics of the cornea and the lens which are usually focused at distance upon dilation.

Fundus cameras employ an aerial image focusing system that relies on a properly set eyepiece reticle before attempting to focus the camera. The focus control of the fundus camera is used to compensate for refractive errors in the subject eye. Many fundus cameras have additional controls to compensate for refractive conditions such as myopia or astigmatism.

Peripheral fundus photography can be particularly challenging. When the eye is rotated to the desired peripheral field of view, the opening in the pupil appears elliptical, making it difficult to fit the entire illuminating beam within its borders. The off-axis angle also causes the image-forming light rays to pass through a flatter portion of the cornea, which will change focus and cause some distortion.
Correctly adjusting the eyepiece reticle for proper focus is of paramount importance. A popular and commonly taught technique involves adjusting the crosshairs at least three successive times, noting the diopter setting each time, and using the average of these numbers. This technique can be very problematic and is best avoided altogether.

In order to properly focus the fundus camera on a consistent basis, the photographer should relax their accommodation at distance to avoid accommodative shift during photography. The aforementioned average-setting technique actually promotes unnecessary accommodation and inaccurate settings. Each time the photographer looks at the numbers marked on the eyepiece, they accommodate to near, then immediately try to relax at distance before looking through the viewfinder again. Repeating these steps multiple times induces accommodative “gymnastics” and subsequent fatigue that can lead to improper settings when accommodation inevitably drifts during a photographic session. For this technique to work properly, someone other than the photographer should note and record the settings, so the photographer can keep accommodation relaxed at distance the entire time.
The best strategy is to ignore the eyepiece numbers altogether, but pay constant attention to the crosshairs and image of the retina. As long as the crosshairs and the aerial image of the fundus both appear sharp at capture, the focus will be correct in a system that is properly calibrated for parfocality.
Viewing lamp brightness can also affect our ability to focus. The brighter the view, the easier it is to focus accurately. Unfortunately, viewing levels that promote good focus can be uncomfortable for the patient, adversely affecting their ability to cooperate. Briefly turning the lamp up to adjust focus, and then dropping it back down to a more tolerable level, is a simple technique that can help both photographer and patient.

Alternately, a green filter can be used as a focusing aid. Because the spectral sensitivity of the human eye peaks in the yellow-green portion of the spectrum, a green filter improves the overall contrast and visibility of the fundus at brightness levels that remain comfortable for the patient. After focusing with green light, the filter is removed from the light path just before exposure. If the fundus camera is equipped with an astigmatic correction device, it can be used to improve focus in patients with significant astigmatism or when photographing peripheral fields.
Digital Imaging
Perhaps the most significant technological change since the introduction of the electronic flash tube has been the implementation of digital imaging. Digital imaging offers several advantages over film-based fundus photography. It facilitates immediate assessment and adjustment of alignment, focus, and exposure. Spatial resolution in current retinal imaging systems varies from 800 x 600 to over 3000 x 2000 pixels. Resolution comes at a cost in terms of light efficiency. High-resolution digital sensors require more light for proper exposure, necessitating an increase in flash settings. Most color sensors do an excellent job in capturing a full spectrum of color for general pictorial use, but often have a difficult time accurately rendering subtle color differences in the red- yellow range.

Another disadvantage to digital imaging is the linear response and narrow exposure latitude of currently available digital sensors. Even the slightest amount of over or under exposure can be detrimental to digital image quality. Proper exposure is essential to obtain adequate color reproduction. Carefully monitor exposure and adjust the flash power up or down as needed with each patient.
Stereo Imaging
Stereo images enhance diagnostic information by providing a visual sense of depth and realism beyond ordinary two-dimensional photographs and are particularly useful in identifying the anatomic location of pathologic findings.

A lateral shift of the fundus camera between sequential photographs causes the illuminating beam of the fundus camera to fall on opposite slopes of the cornea. The resulting cornea-induced parallax creates a hyper-stereoscopic effect that is evident when viewing the stereo pair. Stereo imaging remains the standard protocol for many clinical trials investigating treatment of retinal diseases.
Non-Mydriatic Retinal Cameras and Telemedicine

Non-mydriatic digital fundus cameras are increasingly being used in a variety of clinical settings, often as screening devices for diabetic retinopathy and glaucoma. Non-mydriatic fundus cameras are designed with an infrared focusing system that promotes physiologic dilation in a darkened environment, making them simple to operate. They can be placed at remote primary care sites and operated by available clinical personnel such as nurses and medical assistants. In a telemedicine environment, images are electronically transferred to a centralized reading center for image review and treatment recommendations. Image quality can be quite good, but doesn’t match the quality produced with a mydriatic camera through pharmacologically dilated pupils.